
More than three months into a historic mass immunization effort that has involved thousands of hours of exhaustive planning, many COVID-19 vaccine clinics are running like clockwork, thanks in large part to pharmacy leadership behind the scenes.
 Though not without some pain points — pharmacists say supply has been a source of continuing frustration — the experience and expertise provided by pharmacy staff has been integral to immunization efforts.
Though not without some pain points — pharmacists say supply has been a source of continuing frustration — the experience and expertise provided by pharmacy staff has been integral to immunization efforts.
Even before the arrival of the first COVID-19 vaccines authorized for emergency use in mid-December, the pharmacy teams at Michigan Medicine, University of Iowa Hospitals & Clinics, and Parkland Health and Hospital System in Dallas were vital parts of interdisciplinary teams tasked with ensuring an effective and safe COVID-19 vaccine rollout.
“Pharmacy got critically involved at the beginning of the COVID-19 effort because of all of the logistics with storage, transport, and distribution, so we took a lead role from the very beginning,” said Lindsey Clark, pharmacy manager at Michigan Medicine. “This was a great chance for our pharmacy department to really shine within the organization.”
 Clark said in addition to ordering an ultra-cold freezer back in September in anticipation of the Food and Drug Administration acting swiftly to issue emergency use authorizations for COVID-19 vaccines, the pharmacy team also was involved in site visits to scout out locations for mass vaccination clinics. Michigan Stadium, which can support up to 2,000 vaccinations per day, was selected. As of March 23, nearly 80,000 doses had been administered through Michigan Medicine.
Clark said in addition to ordering an ultra-cold freezer back in September in anticipation of the Food and Drug Administration acting swiftly to issue emergency use authorizations for COVID-19 vaccines, the pharmacy team also was involved in site visits to scout out locations for mass vaccination clinics. Michigan Stadium, which can support up to 2,000 vaccinations per day, was selected. As of March 23, nearly 80,000 doses had been administered through Michigan Medicine.
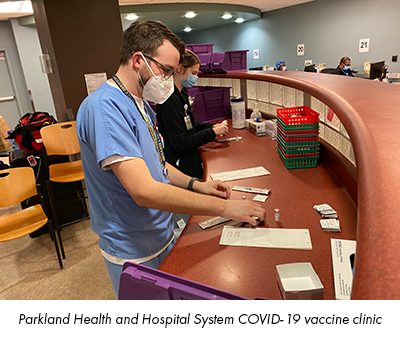
In Texas, where any adult will become eligible for a vaccine on March 29, Parkland has four sites, including two drive-through locations where people can receive a COVID-19 vaccine. As of mid-March, the health system had surpassed 170,000 vaccinations.
 Vivian Bradley Johnson, senior vice president of clinical services, said Parkland didn’t have an established, dedicated vaccine clinic, so they had to build one.
Vivian Bradley Johnson, senior vice president of clinical services, said Parkland didn’t have an established, dedicated vaccine clinic, so they had to build one.
“We started out really focusing on the handling, and making it available and distributing it to the vaccine clinic, and now we’re involved in every aspect, serving as leaders or managers over the vaccine clinic,” Johnson said.
Johnson said the need for more vaccinators was identified quickly, and pharmacy students and retired pharmacists were able to get involved.
“This really showed how valuable our pharmacists are, just by the fact that we are the ones who are doing the dilutions, we are handling the vaccines, keeping tracking of inventory – people don’t know behind the scenes what it takes to keep up with that inventory. It is not that simple.”
Additionally, the pharmacy team has conducted extensive training to staff to ensure the clinics are running smoothly.
 Parkland used a social vulnerability risk index together with a proximity index, which shows how close an individual is to active COVID-19 cases, to prioritize patients for vaccination, said Carrie Berge, vice president of pharmacy services at Parkland, a safety net hospital. A community needs assessment also was conducted to prioritize zip codes with the highest socio-economic needs. Additionally, some patients may not know how to log into their electronic charts for their vaccine appointment, so COVID-19 vaccines may be offered at community clinics.
Parkland used a social vulnerability risk index together with a proximity index, which shows how close an individual is to active COVID-19 cases, to prioritize patients for vaccination, said Carrie Berge, vice president of pharmacy services at Parkland, a safety net hospital. A community needs assessment also was conducted to prioritize zip codes with the highest socio-economic needs. Additionally, some patients may not know how to log into their electronic charts for their vaccine appointment, so COVID-19 vaccines may be offered at community clinics.
“You definitely get more throughput when you have these larger sites than community clinics, but not all of our patients are able to navigate the complex … MyChart functionality. That’s difficult for a lot of people to navigate,” Berge said. “The community clinics are great because they come in for a visit and you can offer them the vaccine. You have to find other avenues to make sure qualifying patients can access the vaccine.”
 Berge said thanks to Parkland’s deep roots in the Dallas community, they are able to work with local media and community and religious organizations to increase awareness about vaccine availability and eligibility.
Berge said thanks to Parkland’s deep roots in the Dallas community, they are able to work with local media and community and religious organizations to increase awareness about vaccine availability and eligibility.
Efforts to improve vaccine confidence have been ongoing, Johnson added.
“We know that we still have hesitancy in our community, and we are doing town halls almost every week, doing media interviews, always trying to help influence people to accept it, Johnson added.
Pharmacy has also been extensively involved in public awareness campaigns in Iowa City. Mike Brownlee, chief pharmacy officer at University of Iowa Hospitals & Clinics (UIHC), said he has done a number of video Q&A sessions for Iowa residents on social media, helping to answer questions and “take the fear level down.”
He is also working with University of Iowa’s dean for diversity, equity, and inclusion on efforts to ensure underserved populations have easy access to COVID-19 vaccines; discussions with city and county officials are underway to set up a clinic.
 Reflecting on UIHC’s COVID-19 vaccination effort, and pharmacy’s leadership throughout, Brownlee said the vaccine rollout and having a seat at the table within the organization has served as a valuable way to highlight what pharmacists are capable of.
Reflecting on UIHC’s COVID-19 vaccination effort, and pharmacy’s leadership throughout, Brownlee said the vaccine rollout and having a seat at the table within the organization has served as a valuable way to highlight what pharmacists are capable of.
“At the local level, our pharmacy team has clearly minimized waste, maximized the number of doses that we can give to individuals, and managed every aspect from storage to clinical guidelines to electronic health records. As a pharmacist and a member of our senior leadership team, I’ve also been able to oversee all pharmacy aspects, as well as the billing process, marketing and communications, the patient experience – the entire process,” Brownlee said.
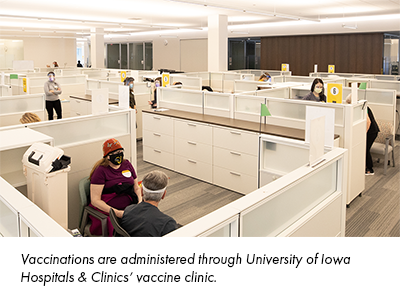
 Brownlee said they took extra care to prioritize the patient experience for UIHC’s vaccine clinic, open to UIHC patients based on eligibility and risk level. When they transformed a large IT building into their large-scale vaccination site, capable of administering up to 4,000 doses per day, they took the time to confirm there would be no bottleneck for patients, arranging for sufficient parking and calculating the number of cars per hour that the site could accommodate.
Brownlee said they took extra care to prioritize the patient experience for UIHC’s vaccine clinic, open to UIHC patients based on eligibility and risk level. When they transformed a large IT building into their large-scale vaccination site, capable of administering up to 4,000 doses per day, they took the time to confirm there would be no bottleneck for patients, arranging for sufficient parking and calculating the number of cars per hour that the site could accommodate.
“Don’t miss the details of the experience for the patient,” Brownlee advised.
Asked about the role of hospitals and health systems in the COVID-19 vaccine rollout, Brownlee said he believes a blend of health system and retail or community pharmacy is important for patients.
“Especially in a state like Iowa that is so rural, having your retail pharmacies have access to vaccine and providing it to the communities is really important,” Brownlee said. “Hospitals and health systems are set up to be amazing mass vaccination sites and they were underutilized for that, from my perspective. The logistics around the vaccine are so difficult that that’s where the health systems do really well to identify at-risk patients to have a proactive approach.”
 Stanley Kent, chief pharmacy officer at Michigan Medicine, said if the COVID-19 vaccine becomes an annual immunization like the flu shot, health systems would definitely play a prominent role.
Stanley Kent, chief pharmacy officer at Michigan Medicine, said if the COVID-19 vaccine becomes an annual immunization like the flu shot, health systems would definitely play a prominent role.
“I think this past six-month period has been a tremendous learning experience. We definitely have the expertise and the capacity, if you will, to administer a lot of vaccine,” Kent said, adding that the daily reporting requirements related to inventory have been labor-intensive. “I can’t imagine that every provider out there would have the time or wherewithal or personnel to do all this. “
Kent said this has been one of the most intensive work efforts he has been a part of, accompanied by a lot of stress.
“I would imagine it would almost be like dealing with a disaster — even though this was not a disaster, it was a good thing — I did get a sense of, this must be a little of what it was like for people working a natural disaster,” he said. “But all in all, it’s been a great experience.”
For more information, ASHP’s recently published resource and infographic outline the essential elements of successful mass immunization programs and emphasize evidence-based, best practices in the safe handling and preparation of vaccines for mass administration.








